Module 7
Oxygen Therapy
OVERVIEW
EVERYBODY IS DEPENDENT ON OXYGEN. Oxygen makes up 21% of the air we breathe, along with nitrogen (78%) and carbon dioxide (less than 1%). Our body relies on a certain blood oxygen level for cells to function properly and sustain life.
By the end of this module, you will have met the following goals:
Goal 1: Learn about oxygen therapy and long-term oxygen therapy (LTOT)
Goal 2: Learn tips for staying active when using long-term oxygen therapy
Goal 3: Exercise with us three times, increase your strength training and continue the home walking program
Goal 4: Take Action to review your oxygen therapy prescription and to create or review your maintenance and back up plans for your oxygen needs
Medical oxygen is a prescription drug in Canada.
Your prescription is based on your needs for achieving and maintaining a healthy blood oxygen level. It is important for you to use your oxygen as prescribed by your healthcare provider.
Too much or too little oxygen could be harmful.
General information
Breathing is an involuntary process that gets oxygen into, and carbon dioxide out of, your lungs. The air sacs in your lungs (the alveoli) are where the oxygen we breathe enters our blood. Breathing is controlled by your brain, which regulates the rate (how often), depth and rhythm of your breathing based on your body’s needs at the time.
When you exert yourself by getting up and out of a chair, putting groceries away, or going up a hill or flight of stairs, your muscles require more oxygen. Your body responds by changing how you breathe so that you can get extra oxygen to the muscle cells that are demanding it. For most people, taking a short break allows them to get their breathing under control.
Many people who live with chronic lung disease have poor gas exchange in the alveoli of their lungs, which causes low blood oxygen level. Depending on your lung disease and its severity, low oxygen levels can occur when you are active, at rest, and/or during sleep.
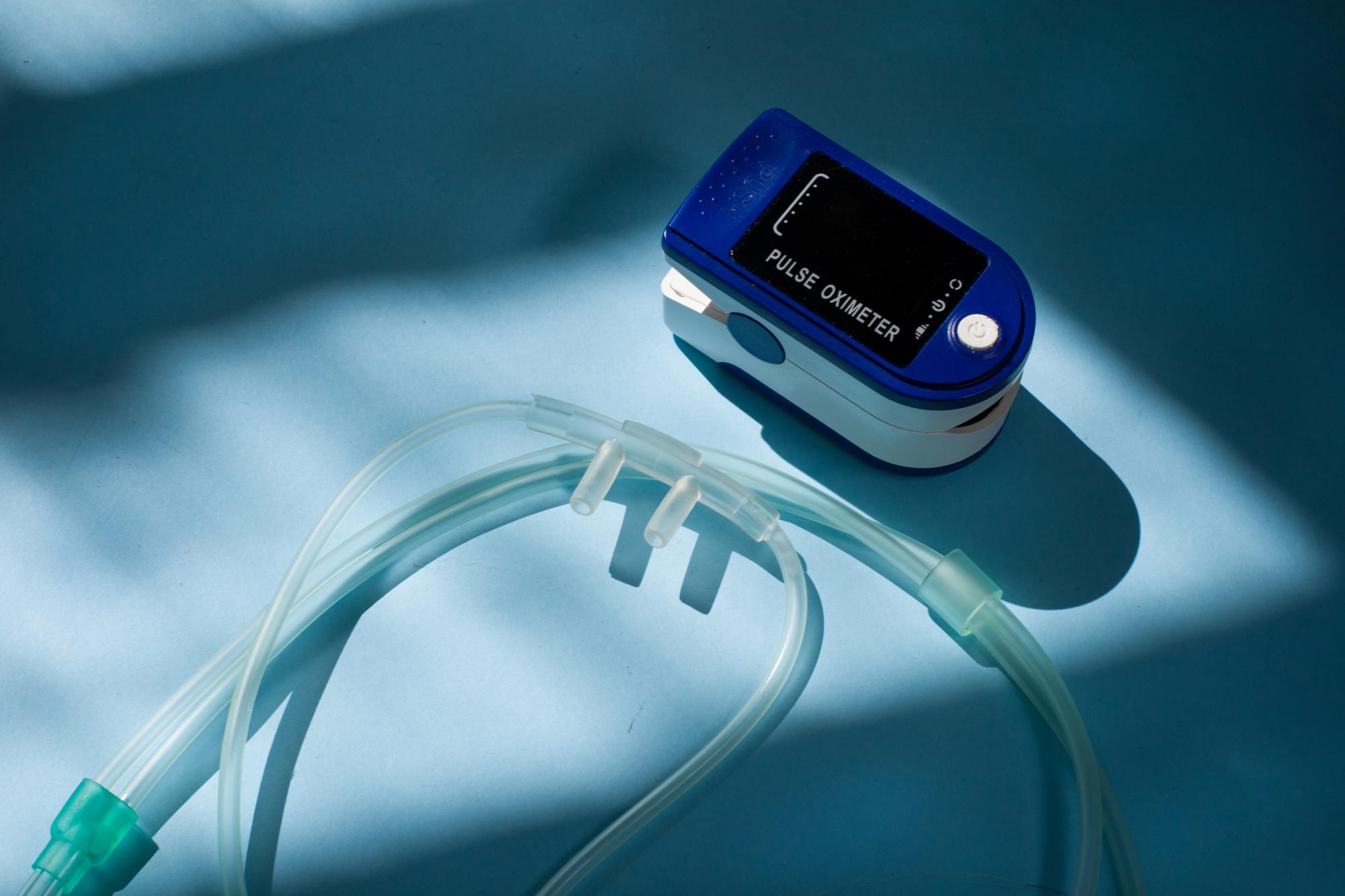
Your healthcare provider can assess your blood oxygen level by asking you to perform a walk test or sit-to-stand test during an office visit. Your blood oxygen level can be measured by an instrument called a pulse oximeter. An infrared light in the oximeter probe that is placed on your finger measures the blood oxygen saturation level, SPO2 (S= saturation, P=pulse, O2= oxygen). A blood test can also be used to measure blood oxygen level. This test is called an arterial blood gas (ABG). Pulse oximeter measures only oxygen saturation (SPO2) but ABG can measure blood level of both oxygen and carbon dioxide.

Not everyone who is short of breath has a low blood oxygen level. Oxygen therapy only benefits people with low blood oxygen levels. Proper assessment is the key.
When blood oxygen levels are low, oxygen therapy helps your lungs, heart and muscles work more comfortably and effectively. Oxygen therapy can improve:
- functional activity
- mood or stress level
- energy level
- concentration
More benefits of oxygen therapy include improved sleep, faster recovery from illness and fewer hospital admissions.
Oxygen prescriptions
Based on your disease severity and your needs, oxygen might be prescribed for you during specific times or continuously throughout the day and night. Your healthcare provider should assess your oxygen needs at rest and with exertion to determine if your oxygen needs. Chronic lung disease is treatable, but not curable. This means that as your disease progresses, your oxygen needs may change. It is very important to assess your blood oxygen level yearly, and to follow the oxygen delivery flow rates prescribed by your healthcare provider.
Oxygen prescriptions should be written to maintain a specific level of blood oxygen saturation, for example: oxygen setting of 2-4 lpm (liters per minute) to maintain oxygen saturation of greater than 90%.
Long-term oxygen therapy
Long-term oxygen therapy (LTOT) is oxygen therapy that is prescribed for at least 15 hours per day. LTOT increases survival and improves quality of life for people with COPD. It also improves quality of life for other lung diseases. LTOT can be delivered through different systems such as compressed oxygen gas cylinders, liquid oxygen or oxygen concentrators.
Compressed oxygen gas /liquid oxygen gas
Compressed oxygen gas /liquid oxygen gas offers non-stop oxygen flow while you inhale and exhale. It’s important to understand that when you get short of breath, for example when you exercise, your breaths become faster and shallower and you may not receive enough extra oxygen. This is why your healthcare provider may recommend that you increase your oxygen flow rate when exercising. Some people wonder why they need oxygen while they sleep – sometimes your blood oxygen level drops because of shallow breathing. Having a prescription for night time oxygen helps you feel better rested and clearer minded when you wake up. (This is different than sleep apnea)
Oxygen-conserving devices: Intermittent oxygen flow devices or pulsed-delivery devices
Special attachments or regulators can be used that deliver oxygen only when you inhale. These devices can deliver a big burst of oxygen when you first inhale then taper down until you exhale, or they can deliver a steady stream of oxygen only during the inhalation of your breath. These systems allow your oxygen delivery devices to last two to four times longer, which means that you can carry smaller devices. These devices are not for everyone. Your healthcare provider will know if this is the right device for you.
Oxygen equipment
Stationary oxygen-delivery equipment
Home oxygen concentrators work by filtering nitrogen out of the air in the room and concentrating the oxygen for delivery to you through your nasal cannula or oxygen mask. Home oxygen concentrators require a power source to operate. You will need a back-up source of oxygen in the event of a power outage.
Freestanding oxygen cylinders or tanks should be considered as a back-up source of oxygen in the event of a power failure. It is very important that all oxygen cylinders or tanks be properly secured for your safety.

Portable oxygen-delivery equipment
Portable oxygen concentrators are lightweight machines that can be carried outside of the home. These devices filter out the nitrogen from the air and concentrates the oxygen for delivery to you based on your prescribed flow rate. Portable concentrators have their own power source. Always carry an extra battery with you.
Portable oxygen cylinders or tanks are smaller cylinders that can be used when leaving the home. This can be carried in a pack, or attached to a walker or wheelchair. Before leaving your home, check how much oxygen is in your tank.
Trans-fill oxygen concentrators or liquid oxygen systems can be used to refill your portable oxygen cylinders from home. Specific training and safety instructions are needed as these devices are tricky to use. Your home medical supply company is responsible for training you.
Supplies
- Nasal cannula, oxygen mask, foam ear pads
- Humidifier: humidification of oxygen delivered for LTOT makes breathing more comfortable and keeps delicate nose and lung tissue healthier. Only use distilled water in a humidifier
Tips for oxygen therapy
- Keep the contact information of your oxygen delivery company with your other important medical information.
- Plan before you go out. See how much oxygen is left in your tank. Check your battery life. Bring extra.
- Make sure your nasal cannula or mask is cleaned with warm soapy water 2 times a week. Replace your cannula every 2 to 4 weeks, or more often if needed.
- If your nose and lips become dry from oxygen use, use water-based lotions. Water-based lotions, moisturizers and lubricants have water as their first ingredient. Avoid products that contain petroleum jelly or oils.
- Saline nasal spray can give your nostrils some relief from dryness.
- Use gauze or foam pads behind your ears if the skin becomes raw.
You can find out more about oxygen therapy in our Oxygen and COPD booklet.
Long-term oxygen therapy does not tie you down, it helps you remain active. When first prescribed, many people feel self-conscious about using their oxygen in public; however, this is usually short lived. Most find that the benefits of using oxygen outweigh their initial discomfort.
OXYGEN IS FLAMMABLE. This means that it is dangerous around a flame. Oxygen should not be worn while close to a gas stove, wood stove, lighted fireplace, while smoking or around any other sources of heat or open flames.
Travelling with oxygen
Plan ahead at least four weeks before travelling.
Make sure you have these items together:
- A medical release from your provider stating that it is safe for you to travel.
- Your oxygen prescription that lists your flow rate and amount of oxygen you use.
Flying with oxygen
Notify the airline about your oxygen usage and needs. There may be an extra charge if they are supplying you with supplemental oxygen. Know the make and model of your portable concentrator, the types of batteries you need and how to manage the alarms. If you need to bring extra tanks, ask the airline about their rules for packing tanks. Ask what to do if there is a layover, as you may need to arrange a supplier to come to the airport.
Going on a cruise with oxygen
Notify the cruise line about your oxygen usage and needs. You can usually take your own concentrator and tanks, though you will have to arrange for your oxygen to be delivered to the ship before departing. Make sure that you have enough oxygen for the entire cruise including ship time and shore time.
Taking a train or bus with oxygen
Notify the bus or train line that you will be travelling with oxygen. Some may have weight limits, but you can take your own tanks and concentrators. To refill tanks, make arrangements in the cities where your transportation stops. Always make sure to have back-up batteries and to be seated in a non-smoking car.
For more information, visit Travelling with Oxygen (Alberta Health Services)
For traveling with Air Canada:
Please refer to the Air Canada website or reservation agents for official requirements:
https://www.aircanada.com/ca/en/aco/home/plan/medical-mobility/travelling-with-oxygen.html
Please print Air Canada's Fitness for Travel Form and have your physician complete it on your behalf.
https://www.aircanada.com/content/dam/aircanada/portal/documents/PDF/en/fft.pdf
You must submit this form to Air Canada a minimum of 48 hours prior to flying (72 hours for international flights). Please follow the instructions on the website carefully.
EXERCISE
This is the week to increase your strength training.
Your steps to success
-
Use your pulse oximeter to check your oxygen saturation and heart rate. If they are normal for you, plan to exercise with us.
-
If you use oxygen, is it set correctly to begin exercising?
-
Are you assessing your symptoms daily?
-
Are you taking your controller inhalers as prescribed, at the same time? Are breathing exercises helping you overcome shortness of breath associated with exertion?
-
Are you using your fast-acting reliever medications 15-20 minutes before exercising? Are you using it less often?
-
Have you eaten? Food can help your mood and your energy. Good food energy in = good exercise energy out.
-
If you quit smoking in Module 4, you have been smoke-free for 3 weeks! Excellent!!
-
You are so close to the end of this program, keep it up! You should feel proud, and capable of meeting new challenges!
-
You will want to start looking for community programs to support continued exercise. Mall walking groups, community centers, gym facilities or in-person pulmonary rehab programs.
Method for exercise progression
Add 2 repetitions during each strength exercise (ie: if you were doing 10 reps, do 12, if you were doing 12 reps, do 14). The max number of reps is 15.
If you were doing 15 repetitions, increase the amount of weight you are using. Add 0.5 – 1kg for strength exercises. Begin with 8 reps of the new weight.
Gradually increase how long you walk, cycle or swim. Below is a guide to help you increase your walking time.
Home walking program
Week 1
5 minutes, 5 times per day
Weeks 2 & 3
10 minutes, 3 times per day
Weeks 4 & 5
15 minutes, 2 times per day
Week 6
20 minutes, 1 time per day
Week 7
25 minutes, 1 time per day
Week 8
30 minutes, 1 time per day
Relaxation, Meditation and Better Breathing
Reinforcing relaxation and diaphragmatic breathing.

Youtube supports many free Mindful Meditation and Better Breathing videos to promote effective breathing techniques, as well as mood, motivation, relaxation, stability, clarity and sleep enhancement. The Canadian Lung Association does not endorse the use of any particular or specific website or channel for meditation and relaxation. Sites listed are suggestions only.
TAKE ACTION
Details of your oxygen prescription
Record the details of your oxygen prescription with this form.
Equipment maintenance
Keeping my equipment clean helps to prevent flare-up of my chronic lung disease symptoms.
Maintenance for my oxygen concentrators
- There are many types of oxygen concentrators. Follow the manufacturer’s recommendations for regular cleaning and yearly maintenance service appointments.
- Keep your concentrator away from corners and walls. This is where dust collects.
- Only distilled water should be used in disposable oxygen humidifier bottles.
- Check the air intake filters twice a week. Make sure they are clean and clear of debris. Do not use soap when cleaning filters.
- Wipe the exterior of the concentrator with a damp cloth and mild cleaner while the concentrator is unplugged.
Maintenance for my nasal cannula/mask
- Wipe my nasal cannula/mask tubing daily with warm water and mild soap, dry well.
- Wipe my extension tubing weekly with warm water and mild cleaner. There is no need to disconnect it from concentrator or from cannula/mask tubing.
- Check for cracks in my nasal cannula/mask and tubing.
- Replace my nasal cannula, mask or tubing every two to four weeks, depending on how you use your oxygen.
- Talk with a certified respiratory educator for more guidelines.
My back-up plan
I have an oxygen cylinder in case of a power outage and know how to use it.
If not, I will contact my oxygen supply company.
I keep extra distilled water for my oxygen concentrator’s humidifier.
If not, I will contact my oxygen supply company.
I have an extra nasal cannula and/or mask, and tubing in case my equipment becomes damaged.
If not, I will contact my oxygen supply company.
I have an extra battery for my portable concentrator.
If not, I will contact my oxygen supply company.
Breathe Better with the Respiratory Care Program
Sun Life and Online Pharmacy, provided by Pillway*, have partnered to offer you and your dependents the Respiratory Care Program. You'll receive 1-on-1 support to help you get back to doing the things you love while breathing easier. The program is available for people living with asthma and chronic obstructive pulmonary disease (COPD), and at no cost.
Read more about the Respiratory Care Program and our collaboration with Sun Life.
Make life more convenient with Online Pharmacy
Online Pharmacy, provided by Pillway*, is an online pharmacy that makes life more convenient by changing the way you get your medications. Offering fast and free delivery, pharmacist support and medication management.
Read more about Online Pharmacy and our collaboration with Sun Life.
*SHG Pharmacy Inc. and SHG West Pharmacy Inc., doing business as Pillway pharmacies, are partially owned by Simpill Health Group Inc. For your information, and as a point of disclosure, Sun Life Assurance Company of Canada has partial ownership in Simpill Health Group Inc.
Programs not available in Quebec.
CLA is not responsible for content from external links. Read our disclaimer here.
FEEDBACK
Tell us what you think
Modules
Introduction · Module 1 · Module 2 · Module 3 · Module 4
Module 5 · Module 6 · Module 7 · Module 8 · Conclusion

Speak to a certified respiratory educator
Call our Health Information Line at 1-866-717-2673 to speak to a certified respiratory educator. You can also email info@lung.ca.
BreatheSTRONG Program: Medical Disclaimer
Before you begin the BreatheSTRONG program, please read and agree to the medical disclaimer.
Medical Advice Disclaimer, Disclaimer of Warranty and Limitation of Liability
Please read this document carefully. The Canadian Lung Association (CLA) strongly recommends that you consult your physician or other qualified healthcare provider before choosing to take part in BreatheSTRONG. You acknowledge that CLA offers no medical assessment, diagnosis, or treatment, and that CLA makes no determination as to whether or not you are physically fit to participate in this program. This program is intended for Canadians living with chronic lung disease, be it obstructive or restrictive in nature. This program is not supervised and therefore not intended for Canadians who are awaiting lung transplant, lung volume reduction surgery or those who have pulmonary hypertension. Certain pre-existing non-respiratory conditions may also exclude you from participating in the exercise portion of this program.
THERE ARE POTENTIAL RISKS INHERENT in your participation in BreatheSTRONG, including, without limitation, worsening of your existing symptoms, an increased load on the heart, episodes of light headedness, fainting, dizziness, pain, chest discomfort, shortness of breath and bone and muscular injury. If you experience faintness, dizziness, pain, or unmanageable shortness of breath at any time while participating in exercise program, you should stop immediately.
CLA and BreatheSTRONG cannot respond to medical emergencies. If you think you have a medical emergency, call 911 immediately.
CLA assumes no liability or responsibility for the use of any information provided by BreatheSTRONG, or for your reliance on this information in place of specific medical advice from a qualified healthcare provider. As is, the health information content provided in this program is current, reviewed and approved by qualified healthcare professionals. To the maximum extent permitted by applicable law, CLA disclaims all liability for any errors or other inaccuracies in the information provided. In no event shall CLA be liable for damages of any kind, including but not limited to direct, indirect, special, consequential, or other monetary damages in connection with your use of or reliance upon information provided by BreatheSTRONG.
By following this program, you acknowledge that you have read, understand and agree to abide by the above Medical Advice Disclaimer, and Disclaimer of Warranty and Limitation of Liability.

